What Is Fungal Acne? Symptoms, Causes, and Treatment Guide
If you’ve been battling tiny, itchy bumps that won’t respond to your usual acne treatments, you might be dealing with something completely different. Fungal acne isn’t actually acne at all—it’s a yeast infection that mimics acne so well, even dermatologists sometimes need a second look. Understanding what you’re really dealing with is the first step toward finally getting clear skin.
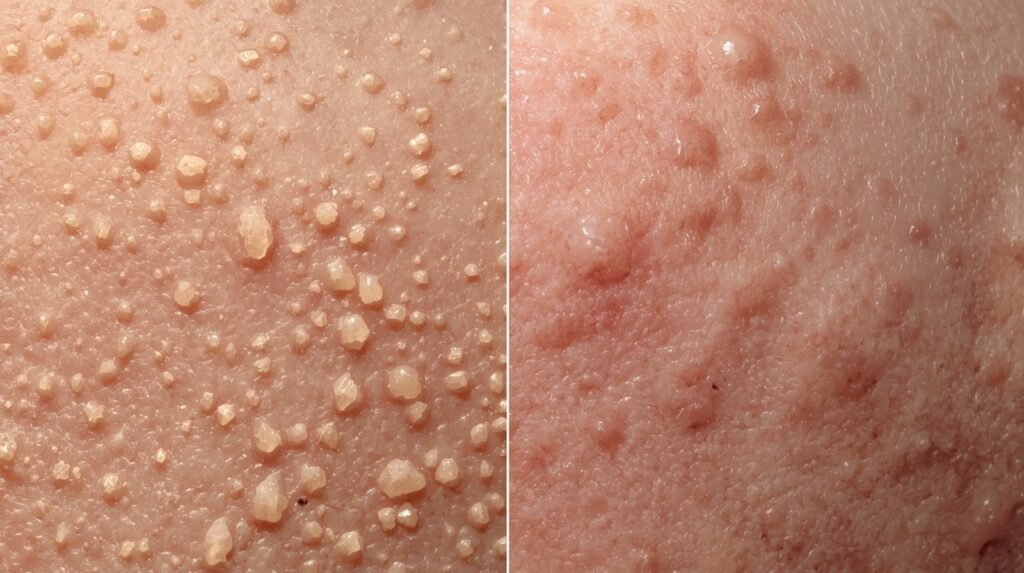
What Is Fungal Acne?
Here’s the truth: “fungal acne” is actually a bit of a misnomer. The medical community calls it Malassezia folliculitis or Pityrosporum folliculitis, and it’s caused by an overgrowth of yeast—not bacteria like traditional acne.
Let me explain it simply. Your skin is home to millions of microorganisms, including a yeast called Malassezia. Normally, this yeast minds its own business, living peacefully in your hair follicles. But when conditions get just right (or wrong, depending on how you look at it), this yeast goes into overdrive and multiplies like crazy inside your follicles, causing inflammation and those frustrating little bumps.
Medical Name: Malassezia Folliculitis
The term “Malassezia folliculitis” tells you exactly what’s happening. Malassezia is the yeast responsible, and folliculitis simply means inflammation of the hair follicles. Some doctors still use the older term “Pityrosporum folliculitis,” which refers to the former name of the yeast. Either way, they’re talking about the same condition.
The Role of Yeast in Fungal Acne
Unlike bacterial acne where Cutibacterium acnes (formerly P. acnes) is the culprit, fungal acne is all about yeast overgrowth. Malassezia feeds on the oils your skin produces, particularly in areas with lots of sebaceous glands. When your skin gets extra oily, sweaty, or humid, it’s like throwing a feast for this yeast—and it multiplies rapidly, triggering that inflammatory response we see as bumps.
Fungal Acne vs Regular Acne: Key Differences
I’ve lost count of how many people I’ve seen who spent months treating fungal acne with benzoyl peroxide and salicylic acid, wondering why nothing was working. The reason? They were fighting the wrong enemy.
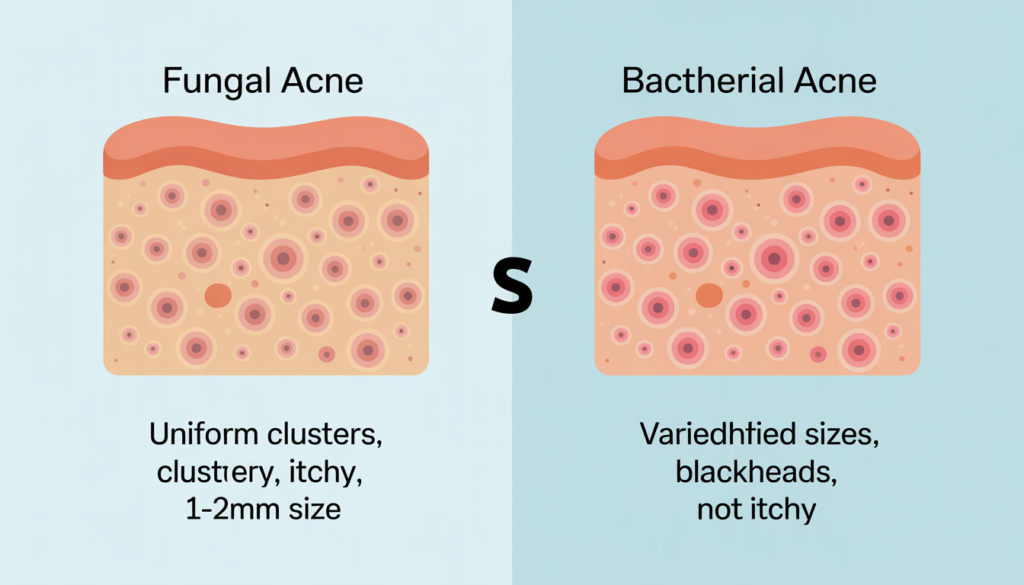
Bacterial Acne vs Fungal Acne
Bacterial acne happens when your pores get clogged with dead skin cells and oil, creating a perfect environment for bacteria to thrive. You’ll see a variety of lesions—blackheads, whiteheads, papules, cysts, and nodules of different sizes.
Fungal acne, on the other hand, shows up as uniform small bumps, typically 1-2mm in size, appearing in clusters. They’re remarkably consistent in appearance, almost like someone scattered identical tiny bumps across your skin. And here’s the kicker: they itch. Sometimes intensely. Regular acne? Not itchy, usually painful instead.
Why Traditional Acne Treatments Don’t Work
This is where things get frustrating. You can slather on all the benzoyl peroxide you want, but you’re not going to kill yeast with antibacterial ingredients. In fact, oral antibiotics—commonly prescribed for severe acne—can actually make fungal acne worse by killing the good bacteria that normally keep yeast in check.
I’ve seen this scenario play out countless times: someone goes on antibiotics for their “acne,” and suddenly they’re dealing with an explosion of itchy bumps. That’s often fungal acne rearing its head.
Can You Have Both Types Simultaneously?
Absolutely, and this is what makes diagnosis tricky. You can have regular acne and fungal acne at the same time, especially on your face. You might have some deeper cystic acne on your cheeks while dealing with clusters of fungal acne on your forehead. Fun times, right?
This is exactly why seeing a dermatologist matters. They can identify which is which and create a treatment plan that addresses both.
Symptoms and Signs of Fungal Acne
Recognizing fungal acne is half the battle. Once you know what you’re looking for, it becomes much easier to spot.
Visual Appearance: Clusters of Small Bumps
The hallmark of fungal acne is its uniformity. Imagine someone took a stamp and pressed it repeatedly on your skin—that’s how consistent these bumps look. They appear in clusters, not scattered randomly like bacterial acne.
Itching and Burning Sensations
If your “acne” itches like crazy, especially when you’re sweating or after a workout, that’s a huge red flag for fungal acne. The itching can be intense enough to disrupt your sleep or make you constantly want to scratch. Regular acne might be tender or painful, but it rarely itches.
Uniform Size and Shape Characteristics
Most fungal acne bumps measure between 1-2mm—tiny, consistent, and monomorphic (meaning they all look the same). You won’t see the variety you’d get with bacterial acne, where you might have everything from tiny whiteheads to large, inflamed cysts.
Red Bumps and Pustules
Fungal acne typically presents as small red papules (bumps without pus) or pustules (white-headed bumps with pus). Sometimes you’ll see a red ring around each bump. They can develop quickly—like, you wake up and suddenly have a whole crop of them.
What Causes Fungal Acne?
Understanding what triggers fungal acne can help you prevent it from happening in the first place. Let’s break down the main culprits.
Malassezia Yeast Overgrowth
At its core, fungal acne happens when Malassezia yeast populations explode beyond normal levels. This yeast is lipophilic, meaning it loves fat and oil. It thrives on sebum, which is why you’ll often see fungal acne in oilier areas of your body.
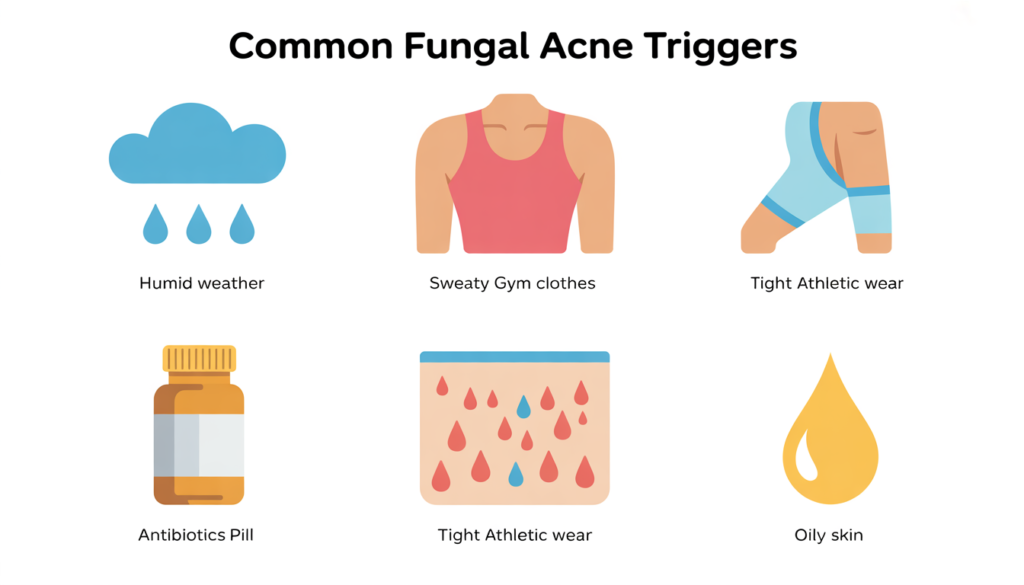
Hot and Humid Environment Factors
If you live in a tropical climate or somewhere with sweltering, humid summers, you’re at higher risk. Heat and humidity create the perfect breeding ground for yeast. I’ve noticed that people often get their first fungal acne outbreak after moving to a warmer climate or during an unusually humid summer.
Excessive Sweating and Moisture
Athletes, gym enthusiasts, and anyone who sweats heavily are prime candidates for fungal acne. That’s because yeast absolutely loves warm, moist environments. If you’re sitting in sweaty workout clothes for hours or working in conditions that make you perspire constantly, you’re giving Malassezia exactly what it needs to proliferate.
Antibiotic Use and Yeast Imbalance
Here’s something your doctor might not tell you: oral antibiotics are one of the biggest triggers for fungal acne. Antibiotics kill bacteria—including the beneficial bacteria that keep yeast populations under control. Remove that competition, and yeast can multiply unchecked.
I’ve seen this happen so often with people on long-term antibiotic therapy for acne. They start seeing improvement in their bacterial acne, then suddenly develop these itchy clusters of bumps. That’s fungal acne taking advantage of the bacterial vacuum.
Weakened Immune System Impact
If your immune system is compromised—whether from illness, certain medications like steroids, or conditions like diabetes—you’re more susceptible to fungal infections of all kinds, including fungal acne. Your body’s natural defenses that normally keep yeast in check aren’t working at full capacity.
Tight Clothing and Trapped Moisture
Those cute, form-fitting workout clothes? They might be contributing to your fungal acne. Tight clothing, especially synthetic fabrics that don’t breathe well, trap sweat and heat against your skin. Add some friction, and you’ve got the perfect storm for yeast overgrowth.
Oily Skin and Sebum Production
People with naturally oily skin or conditions that increase oil production are more prone to fungal acne. Remember, Malassezia feeds on skin oils. More oil means more food for yeast, which means higher likelihood of overgrowth.
Where Does Fungal Acne Appear on the Body?
Fungal acne has its favorite hangout spots, and they’re usually areas where you’re oilier or sweatier.
Face (Forehead, Chin, Temples, Hairline)
On the face, fungal acne loves the forehead, especially along the hairline and temples. The chin gets hit pretty frequently too. These areas tend to be oilier and can trap sweat under hair or hats.
Chest and Upper Torso
The chest is probably the most common location for fungal acne. If you’re seeing clusters of itchy bumps across your upper chest, particularly if they appeared after exercise or during summer, fungal acne should be high on your suspect list.
Back and Shoulders
The back and shoulders—especially the upper back—are prime real estate for fungal acne. These areas sweat a lot, especially during workouts, and they’re harder to keep dry and clean throughout the day.
Upper Arms
The upper arms can develop fungal acne, particularly in people who do a lot of upper body workouts or wear tight sleeves that trap sweat.
Neck
The neck is another common spot, especially the back of the neck where sweat can accumulate under hair or shirt collars.
Who Is Most Likely to Get Fungal Acne?
While anyone can develop fungal acne, certain groups are at higher risk.
Adolescents and Young Adult Males
Teenage boys and young men in their twenties tend to get fungal acne more often, likely because they typically produce more sebum and sweat more during physical activities.
People in Hot, Humid Climates
If you live in Florida, the Gulf Coast, Hawaii, or anywhere tropical, you’re playing on hard mode when it comes to fungal acne. The constant heat and humidity are like a yeast incubator.
Athletes and Active Individuals
Anyone who exercises regularly and sweats heavily is at increased risk. This includes runners, cyclists, CrossFit enthusiasts, and anyone doing intense cardio or weight training.
Those with Weakened Immune Systems
People with diabetes, HIV, those undergoing chemotherapy, or taking immunosuppressive medications have a harder time controlling yeast populations naturally.
People Taking Antibiotics
Long-term antibiotic use, especially for acne treatment, significantly increases your risk of developing fungal acne.
Individuals with Hyperhidrosis
If you have a condition that causes excessive sweating (hyperhidrosis), you’re creating ideal conditions for Malassezia overgrowth throughout the day.
How Is Fungal Acne Diagnosed?
Getting the right diagnosis is crucial because the treatment is completely different from regular acne.
Clinical Examination by Dermatologist
An experienced dermatologist can often diagnose fungal acne just by looking at it and asking about your symptoms. The uniform appearance, clustering pattern, itchiness, and location are all telltale signs.
Skin Scraping and KOH Preparation
If there’s uncertainty, your dermatologist might do a quick skin scraping. They’ll gently scrape the top of a few bumps, put the sample on a slide with potassium hydroxide (KOH), and look at it under a microscope. If they see yeast spores and hyphae inside the follicles, that confirms fungal acne.
Microscopic Analysis
Under the microscope, Malassezia has a distinctive appearance—often described as “spaghetti and meatballs” because of the mix of yeast cells and filaments. It’s pretty unmistakable once you know what you’re looking for.
Wood’s Lamp Examination
Some dermatologists use a Wood’s lamp, which is basically a black light, to examine your skin. Certain fungi fluoresce under this light, though this test isn’t always definitive for Malassezia.
Skin Biopsy (When Necessary)
In rare cases where the diagnosis is still unclear, a small skin biopsy might be needed. This involves removing a tiny piece of skin to examine under a microscope. It’s not usually necessary for fungal acne, but it can rule out other conditions.
Treatment Options for Fungal Acne
Now for the good news: once you know you’re dealing with fungal acne, it’s usually pretty straightforward to treat.
Topical Antifungal Treatments
Topical antifungals are the first-line treatment for most cases of fungal acne.
Ketoconazole Cream and Shampoo
Ketoconazole is probably the most commonly recommended treatment. The 2% shampoo (brands like Nizoral are available over-the-counter) can be used as a face and body wash. Leave it on for 5-10 minutes before rinsing—this contact time is crucial for it to work.
I recommend using it 2-3 times per week initially, then reducing to once weekly for maintenance once your skin clears up. The cream formulation can be applied directly to affected areas once or twice daily.
Selenium Sulfide Shampoo
Selenium sulfide shampoo (like Selsun Blue) works similarly to ketoconazole. It’s another dandruff shampoo that doubles as an effective fungal acne treatment. Use it the same way—as a wash that you leave on for several minutes.
Clotrimazole Applications
Clotrimazole is available over-the-counter as an antifungal cream (often sold for athlete’s foot). It can be applied to fungal acne bumps twice daily. It’s gentle and generally well-tolerated.
Econazole Cream
Econazole requires a prescription but is very effective for fungal acne. It’s typically applied once or twice daily to affected areas.
Oral Antifungal Medications
For widespread or stubborn fungal acne, oral antifungals are often necessary.
Fluconazole
Fluconazole (commonly known as Diflucan) is usually prescribed as a single dose or a short course. It works quickly and efficiently, often clearing fungal acne within a couple of weeks. The typical regimen might be 150-200mg once weekly for 2-4 weeks.
Itraconazole
Itraconazole (Sporanox) is another oral option, often prescribed at 200mg daily for 1-2 weeks. It penetrates well into skin tissue and can be very effective for resistant cases.
Over-the-Counter Options
Before you spend money on a dermatologist visit, you can try OTC antifungal shampoos or creams. Many people find success with ketoconazole or selenium sulfide shampoos used as body washes. Just be patient—topical treatments take longer than oral medications.
Photodynamic Therapy (PDT)
For cases that don’t respond to standard treatments, some dermatologists are exploring photodynamic therapy. This involves applying a photosensitizing agent to the skin and then exposing it to specific wavelengths of light. It’s still being studied for fungal acne but shows promise.
Treatment Duration and Expectations
Topical treatments typically take 2-4 weeks to show significant improvement, sometimes longer. Oral antifungals work faster—you might see improvement within a week or two. The frustrating part? Fungal acne tends to recur if you don’t address the underlying triggers.
Most dermatologists recommend continuing treatment for 2-4 weeks after your skin clears to ensure you’ve fully eliminated the yeast overgrowth.
How to Prevent Fungal Acne
Prevention is honestly easier than treatment when it comes to fungal acne. Here’s what actually works.
Proper Hygiene Practices
Wash your face and body twice daily with a gentle cleanser. If you’re prone to fungal acne, consider using an antifungal wash 2-3 times per week as maintenance, even when your skin is clear.
Showering After Exercise
This is non-negotiable. As soon as you finish working out, shower. Don’t sit around in sweaty clothes scrolling through your phone. The longer sweat stays on your skin, the happier yeast becomes.
Wearing Breathable Fabrics
Choose natural, breathable fabrics like cotton over synthetic materials when possible. If you do wear workout clothes made from synthetic fabrics, make sure they’re moisture-wicking and not skin-tight.
Avoiding Tight Clothing
Give your skin room to breathe. Tight clothing creates friction and traps moisture—exactly what you don’t want if you’re trying to prevent fungal acne.
Changing Out of Wet Clothes Quickly
Whether it’s your swimsuit, gym clothes, or work uniform, change out of damp clothing as soon as possible. Don’t rewear workout clothes without washing them first (I know you’ve done it—we all have, but stop).
Using Clean Hot Tubs Only
Poorly maintained hot tubs and pools are breeding grounds for all sorts of fungi and bacteria. If you’re going to use one, make sure it’s properly chlorinated and maintained. And shower immediately afterward.
Proper Shaving and Waxing Techniques
Hair removal can damage follicles, making them more susceptible to yeast invasion. Use sharp, clean razors, shave in the direction of hair growth, and consider using an antiseptic aftershave to prevent infection.
Avoiding Oily Skincare Products
Heavy, oil-based moisturizers and sunscreens can exacerbate fungal acne. Look for non-comedogenic, oil-free products. Gel-based formulations are usually safer if you’re prone to fungal acne.
Managing Environmental Factors

If you live in a hot, humid climate, keep your living space cool and dry when possible. Use air conditioning or fans. If you work in hot conditions, take breaks to cool down and dry off when you can.
When to See a Dermatologist
While you can certainly try OTC treatments first, there are times when professional help is necessary.
Persistent Breakouts Despite Treatment
If you’ve been using OTC antifungal treatments consistently for 3-4 weeks and you’re not seeing any improvement, it’s time to see a dermatologist. You might need prescription-strength medications.
Differentiating from Traditional Acne
If you’re not sure whether you’re dealing with fungal acne, bacterial acne, or both, a dermatologist can diagnose you properly. Using the wrong treatment wastes time and money.
Recurring Infections
If fungal acne keeps coming back despite your best prevention efforts, a dermatologist can help you figure out why and develop a long-term management strategy.
Need for Prescription Medications
Some cases of fungal acne are too widespread or stubborn to treat with OTC products alone. Oral antifungals require a prescription and medical supervision. For those dealing with acne concerns, understanding different acne types is crucial for effective treatment.
Living with Fungal Acne: Management Tips
Managing fungal acne long-term means building the right habits.
Home Remedies and Relief Methods
While home remedies can’t cure fungal acne, they can provide relief. Tea tree oil has antifungal properties and can be diluted and applied to bumps. Apple cider vinegar diluted with water can help restore skin pH. Just don’t use these as substitutes for proven antifungal treatments.
Warm Compress Applications
If your fungal acne is inflamed and uncomfortable, warm compresses can provide temporary relief. Apply a clean, warm washcloth to affected areas for 10-15 minutes a few times daily.
Long-term Management Strategies
Many people need to use antifungal washes 1-2 times weekly indefinitely to prevent recurrence. Think of it like using dandruff shampoo—it’s ongoing maintenance, not a one-time cure.
Keep a bottle of ketoconazole or selenium sulfide shampoo in your shower and use it regularly, especially during summer months or when you’re exercising frequently.
Post-Treatment Hyperpigmentation
After fungal acne clears, you might be left with dark spots (post-inflammatory hyperpigmentation). These typically fade over time, but you can speed up the process with ingredients like vitamin C, niacinamide, or azelaic acid. Just make sure these products are oil-free.
Preventing Recurrence
The key to preventing fungal acne from coming back is identifying and avoiding your specific triggers. Keep a journal if needed. Did your fungal acne appear after starting antibiotics? After a week at the beach? During that humid summer month?
Once you know your triggers, you can be proactive. Start using antifungal washes preventively before your trigger season hits.
Frequently Asked Questions
How do I know if my acne is fungal or bacterial?
Fungal acne appears as small, uniform, itchy bumps in clusters, usually 1-2mm in size and remarkably consistent in appearance. Unlike bacterial acne, you won’t see blackheads or varying sizes of pimples. The itching is the biggest giveaway—if your “acne” makes you want to scratch constantly, especially when sweating, that strongly suggests fungal acne. Bacterial acne tends to be painful rather than itchy and shows more variety in lesion types. If traditional acne treatments with benzoyl peroxide or salicylic acid aren’t working after several weeks, you’re likely dealing with fungal acne, not bacterial.
Can fungal acne go away on its own?
Unfortunately, fungal acne rarely resolves without treatment. Unlike a simple bacterial breakout that might clear up with good hygiene alone, fungal acne requires antifungal medications to eliminate the yeast overgrowth causing the problem. The Malassezia yeast naturally lives on everyone’s skin, so once it’s overgrown, it won’t just decide to retreat on its own. Even worse, without treatment, fungal acne can persist for months or years. The good news is that once you treat it properly with antifungals, it typically clears up relatively quickly—though you’ll need to maintain preventive measures to keep it from coming back.
What triggers fungal acne breakouts?
The most common triggers are hot and humid weather, excessive sweating (especially from exercise), wearing tight or synthetic clothing that traps moisture, using heavy oil-based moisturizers or sunscreens, taking oral antibiotics, and having a weakened immune system. Basically, anything that creates a warm, moist environment on your skin or disrupts the normal balance of microorganisms can trigger fungal acne. I’ve seen people develop it after moving to a tropical climate, starting a new intense workout routine, going on antibiotics for strep throat, or even just using a rich, occlusive moisturizer during summer. Poorly maintained hot tubs and pools are also notorious triggers.
How long does it take to cure fungal acne?
With proper antifungal treatment, you should start seeing improvement within 2-4 weeks, though complete clearance can take longer. Oral antifungal medications like fluconazole work faster—many people notice significant improvement within 1-2 weeks. Topical treatments are slower and might take 4-8 weeks for full results. The timeline also depends on how widespread your fungal acne is and whether you’re consistently using treatments correctly. Here’s the catch: “cure” might not be the right word, because fungal acne tends to recur if you stop prevention measures. Many people need to use maintenance therapy (like antifungal washes 1-2 times weekly) long-term to keep it away.
Can I use regular acne products on fungal acne?
No, and this is a crucial mistake many people make. Regular acne products containing benzoyl peroxide, salicylic acid, or retinoids target bacteria and clogged pores—they do nothing against yeast. In fact, some traditional acne treatments might make fungal acne worse by disrupting your skin barrier or changing the pH in ways that favor yeast growth. You need antifungal treatments specifically—products with ketoconazole, selenium sulfide, clotrimazole, or other antifungal ingredients. That said, if you have both fungal and bacterial acne simultaneously (which happens), your dermatologist might prescribe both types of treatments to use on different areas or at different times.
Is fungal acne contagious?
No, fungal acne is not contagious from person to person. You can’t “catch” it from someone who has it, and you can’t spread it to others. The Malassezia yeast that causes fungal acne already lives on everyone’s skin naturally—it’s part of your normal skin microbiome. Fungal acne develops when this yeast multiplies excessively due to certain conditions like heat, humidity, or moisture, not from contact with someone else’s skin. So you don’t need to worry about sharing towels or hugging someone with fungal acne. That said, you should still avoid sharing personal items like razors or using dirty hot tubs, since those can introduce other types of infections.
What’s the best over-the-counter treatment for fungal acne?
The most effective OTC option is ketoconazole 2% shampoo (brands like Nizoral), which you can find at most drugstores. Use it as a face and body wash, applying it to affected areas and letting it sit for 5-10 minutes before rinsing off. Do this 2-3 times per week initially, then once weekly for maintenance. Selenium sulfide shampoo (like Selsun Blue) works similarly. For targeted treatment, OTC clotrimazole cream (usually marketed for athlete’s foot) can be applied directly to bumps twice daily. The key is consistency and proper contact time—don’t just wash it off immediately. These treatments work, but they’re slower than prescription oral antifungals, so be patient and give them at least 3-4 weeks to show results.
Why does fungal acne keep coming back?
Fungal acne recurs because the Malassezia yeast naturally lives on your skin—it’s part of your permanent skin microbiome. You can clear an overgrowth, but you can’t eliminate the yeast entirely. If you return to conditions that favor yeast growth (hot, humid weather, intense sweating, tight clothes, heavy skincare products), it can multiply again. This is why many people find they get fungal acne every summer, or whenever they ramp up their workout routine, or when they’re on antibiotics. The solution is ongoing prevention: use antifungal washes 1-2 times weekly as maintenance, shower promptly after sweating, wear breathable clothing, and avoid oil-heavy products. Think of it like managing dandruff—it’s controllable with the right routine, but you can’t cure it permanently.
Can diet affect fungal acne?
The connection between diet and fungal acne isn’t as well-established as it is for hormonal acne, but there’s some evidence that foods promoting yeast growth might worsen the condition. High-sugar foods and alcohol can potentially feed Malassezia yeast, though most of this yeast lives on the outside of your body, not in your gut. Some people report improvement when they reduce sugar and alcohol intake, but dietary changes alone won’t cure fungal acne—you still need antifungal treatment. If you want to try dietary modifications, cut back on refined sugars, alcohol, and high-glycemic foods while you’re treating fungal acne. Just don’t expect diet changes to replace proper antifungal therapy. The external factors (sweat, humidity, skincare products) matter much more than internal ones for this condition.
Should I see a dermatologist for fungal acne?
You should definitely see a dermatologist if you’ve tried OTC antifungal treatments for 3-4 weeks without improvement, if you’re not sure whether you have fungal or bacterial acne, if your symptoms are severe or rapidly spreading, or if you experience frequent recurrences despite prevention efforts. A dermatologist can provide accurate diagnosis through clinical examination or testing, prescribe stronger treatments like oral antifungals when needed, and help you develop a personalized prevention strategy. They can also address any post-inflammatory hyperpigmentation left behind after the fungal acne clears. While you can certainly start with OTC treatments, don’t suffer through months of ineffective self-treatment—professional help can save you time, frustration, and potential scarring.
Conclusion
Fungal acne might seem like a confusing, frustrating skin condition, but once you understand what you’re dealing with, it becomes much more manageable. The key is recognizing that those itchy, uniform bumps aren’t regular acne and won’t respond to traditional acne treatments. Armed with the right antifungal treatments—whether OTC shampoos or prescription medications—and smart prevention strategies, you can clear your skin and keep fungal acne from coming back.
Remember, this isn’t about being dirty or doing something wrong. Fungal acne is simply your skin’s reaction to yeast overgrowth under certain conditions. With a bit of knowledge and the right approach, you can win this battle. If you’re struggling to figure out what’s going on with your skin, don’t hesitate to see a dermatologist. Sometimes professional guidance is exactly what you need to finally get clear skin and keep it that way.
