Staring at yet another painful cyst on your jawline the week before your period? You’re not alone—and it’s not your fault. How to treat hormonal acne has become one of the most searched skincare questions for good reason: nearly 50% of women in their 20s and 25% in their 40s struggle with these stubborn, deep breakouts that refuse to respond to typical acne treatments. Unlike the teenage pimples you might remember, hormonal acne plays by completely different rules, showing up on your lower face, jawline, and chin with a vengeance that over-the-counter products simply can’t match. The good news? Once you understand what’s actually happening beneath your skin, you can finally break the cycle.
What is Hormonal Acne?
Definition and Characteristics
Hormonal acne isn’t just a buzzword your favorite skincare influencer throws around—it’s a legitimate medical condition that dermatologists diagnose daily. This type of acne develops when fluctuating hormone levels trigger your oil glands to go into overdrive, producing excess sebum that clogs pores and creates the perfect breeding ground for inflammation.
I’ve seen countless patients walk into my office frustrated because they’ve spent hundreds on products that worked for their friends but did absolutely nothing for their own skin. That’s because hormonal acne requires a fundamentally different approach than regular acne vulgaris.
How Hormonal Acne Differs from Regular Acne
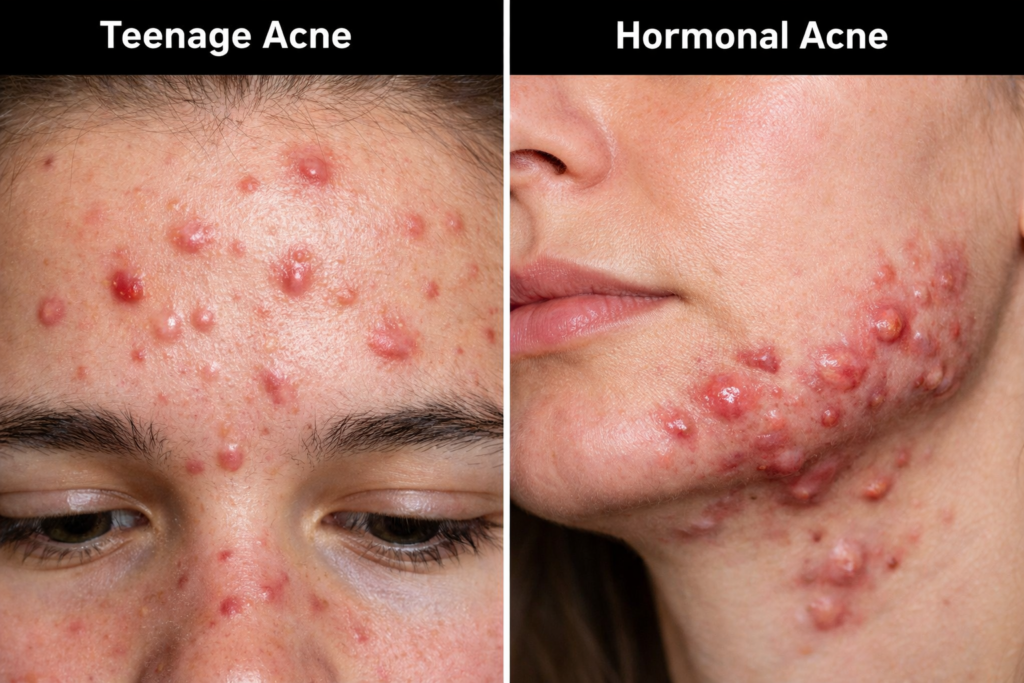
Here’s what sets hormonal acne apart: while typical teenage acne often responds well to benzoyl peroxide and salicylic acid, hormonal acne laughs in the face of these treatments. The root cause isn’t just bacteria or clogged pores—it’s your body’s internal hormonal orchestra playing out of tune.
Regular acne tends to appear across your T-zone (forehead, nose, and cheeks), but hormonal acne has a signature calling card: it camps out along your jawline, chin, and lower cheeks in what dermatologists call a “U-shaped” pattern. These aren’t your average whiteheads either—they’re often deep, painful cysts and nodules that lurk beneath the skin’s surface.
Who Gets Hormonal Acne?
While hormonal acne can technically affect anyone, women bear the brunt of this condition. About 80% of cases occur in adult females, particularly those between 25 and 50 years old. Men aren’t completely off the hook though—they can develop hormonal acne during puberty or if they’re undergoing testosterone treatment.
What’s particularly frustrating is that many women experience what I call “persistent acne”—breakouts that started in their teens and never really left. Others develop “late-onset acne,” which appears for the first time in adulthood, often triggered by life changes like discontinuing birth control, pregnancy, or approaching menopause.
When Does Hormonal Acne Occur?
Timing is everything with hormonal acne. Most women notice a predictable pattern: breakouts appear like clockwork 7-10 days before their period, when progesterone levels spike and estrogen drops. This hormonal shift increases sebum production and inflammation, creating the perfect storm for deep, painful breakouts.
Pregnancy, perimenopause, and menopause are other prime times for hormonal acne to rear its ugly head. Even stress can trigger hormonal acne by elevating cortisol levels, which in turn increases androgen production.
Symptoms and Signs of Hormonal Acne
Where Hormonal Acne Appears
If you’re constantly battling breakouts along your jawline, chin, and lower cheeks, you’re looking at hormonal acne’s favorite real estate. While teenage acne throws a party all over your face, hormonal acne is more selective, targeting areas with high concentrations of oil glands that are particularly sensitive to androgens.
I’ve had patients who never broke out anywhere except their chin—same spot, every month, like clockwork. That predictability is actually a diagnostic clue that helps me identify hormonal acne versus other skin conditions.
Types of Lesions (Blackheads, Whiteheads, Cysts, Nodules)
Hormonal acne presents as a mixed bag of lesion types:
- Blackheads and whiteheads (comedones): Small bumps that may seem relatively innocent but indicate clogged pores
- Papules and pustules: Inflamed red bumps, some with white centers filled with pus
- Nodules: Large, hard bumps deep under the skin that hurt like hell
- Cysts: The worst offenders—deep, pus-filled lumps that can persist for weeks and often leave scars
Cystic hormonal acne is the most severe form, causing significant pain and often leading to post-inflammatory hyperpigmentation, especially in darker skin tones.
Severity Scales and Assessment
Dermatologists use specific tools to assess hormonal acne severity. The AFAST (Adult Female Acne Scoring Tool) was developed specifically for women’s hormonal acne, evaluating both facial acne and the submandibular zone (under the jaw). Scores range from 0 (clear skin) to 5 (severe, widespread inflammation with nodules).
Understanding your severity level helps determine whether you need prescription medication or can manage with topical treatments and lifestyle changes.
What Causes Hormonal Acne
Role of Androgens and Hormones
Let’s talk about the real troublemaker: androgens. These hormones—including testosterone, DHEA, and DHT (dihydrotestosterone)—stimulate your sebaceous glands to produce more oil. Women naturally have lower androgen levels than men, but even small fluctuations can trigger major skin chaos.
Here’s the kicker: you don’t need abnormally high androgen levels to develop hormonal acne. Your skin might just be hypersensitive to normal hormone levels, with sebaceous glands that overreact to even slight hormonal changes.
Hormonal Fluctuations (Menstruation, Pregnancy, Menopause)
Your menstrual cycle creates a monthly hormonal rollercoaster. During the luteal phase (the two weeks before your period), progesterone rises while estrogen drops, creating a relatively androgen-rich environment that increases oil production. This explains why 60-70% of women report acne flares right before their periods.
Pregnancy throws another curveball. While some women experience glowing, clear skin, others develop severe acne during the first trimester when hormone levels surge unpredictably. Postpartum acne is also common as your hormones struggle to recalibrate.
Perimenopause and menopause bring their own challenges. As estrogen levels decline, the relative proportion of androgens increases, triggering breakouts in women who never struggled with acne before.
Polycystic Ovary Syndrome (PCOS) and Endocrine Disorders
PCOS is the elephant in the room when discussing hormonal acne. This endocrine disorder affects 5-10% of women of reproductive age and causes elevated androgen levels, insulin resistance, and irregular periods—all recipes for severe, persistent acne.
If you have hormonal acne plus irregular periods, unexplained weight gain, or excessive facial hair growth, you should get evaluated for PCOS. Other endocrine conditions like thyroid disorders and adrenal hyperplasia can also manifest as hormonal acne.
Stress and Cortisol
Stress isn’t just in your head—it’s on your face. When you’re stressed, your body pumps out cortisol, which triggers a cascade of hormonal changes including increased androgen production. Cortisol also promotes inflammation and can impair your skin’s barrier function, making you more susceptible to breakouts.
I’ve noticed that many of my patients with demanding careers or high-stress lifestyles have the worst hormonal acne, regardless of their skincare routines.
Genetic Predisposition
Genetics load the gun; hormones pull the trigger. If your mom or siblings struggled with adult acne, you’re significantly more likely to develop it too. Your genes influence everything from your sebaceous gland size to how sensitive your skin is to androgens.
Lifestyle and Environmental Triggers
Beyond hormones and genetics, several lifestyle factors can worsen hormonal acne:
- High-glycemic foods: Spike insulin and IGF-1, increasing androgen production
- Dairy products: May contain hormones that stimulate oil glands
- Lack of sleep: Disrupts hormonal balance and increases stress hormones
- Certain medications: Birth control pills with androgenic progestins, steroids, and some psychiatric drugs
- Comedogenic products: Heavy makeup, sunscreens, and hair products that clog pores
Topical Treatments for Hormonal Acne
Retinoids (Tretinoin, Adapalene, Tazarotene)
Retinoids are my first-line topical treatment for hormonal acne, and here’s why they’re so effective: they normalize skin cell turnover, preventing pores from getting clogged in the first place. They also have anti-inflammatory properties and help fade post-acne dark spots.
Tretinoin (Retin-A) is the gold standard prescription retinoid. Start with 0.025% cream and work up to higher concentrations as your skin builds tolerance.
Adapalene (Differin) is available over-the-counter at 0.1% strength and tends to be less irritating than tretinoin, making it great for sensitive skin.
Tazarotene (Tazorac) is the strongest retinoid but also the most irritating—I typically reserve this for stubborn cases.
Pro tip: Always apply retinoids at night and use them consistently for at least 12 weeks before judging results. Many people quit after a few weeks of purging, missing out on the clear skin that’s just around the corner.
Benzoyl Peroxide
While benzoyl peroxide kills acne bacteria effectively, it’s not a magic bullet for hormonal acne when used alone. It works best in combination with other treatments, particularly retinoids. Stick with 2.5-5% concentrations—higher strengths aren’t more effective and will just irritate your skin.
Azelaic Acid
Azelaic acid is an unsung hero for hormonal acne, especially if you struggle with post-inflammatory hyperpigmentation. At 15-20% concentrations, it reduces inflammation, kills bacteria, and helps fade dark spots left behind by previous breakouts.
I particularly recommend azelaic acid for women with darker skin tones who are prone to hyperpigmentation, and it’s safe during pregnancy—a huge plus when many other acne treatments are off-limits.
Salicylic Acid
Salicylic acid is a beta-hydroxy acid that penetrates oil-filled pores to clear out debris. It’s helpful for preventing comedones but isn’t strong enough to treat hormonal acne as monotherapy. Use it in your cleanser or as a spot treatment alongside more potent prescription medications.
Topical Antibiotics (Clindamycin, Erythromycin)
Here’s my honest take on topical antibiotics: never use them alone. Due to widespread antibiotic resistance, topical antibiotics must always be combined with benzoyl peroxide or a retinoid. Products like Benzaclin (clindamycin + benzoyl peroxide) offer this combination in one formula.
Dapsone Gel
Dapsone 5% gel (Aczone) is particularly effective for inflammatory hormonal acne in women. It reduces inflammation without the resistance issues of antibiotics. Apply it twice daily—many patients see improvement within 4-6 weeks.
Combination Topical Treatments
The most effective approach combines multiple mechanisms of action. A typical regimen might include:
- Morning: Cleanser → Azelaic acid → Moisturizer → Sunscreen
- Evening: Cleanser → Tretinoin OR Adapalene + Benzoyl peroxide → Moisturizer
Oral Medications for Hormonal Acne
Oral Antibiotics (Tetracyclines, Doxycycline, Minocycline)
Oral antibiotics can jumpstart your treatment by reducing inflammation quickly, but they’re not a long-term solution for hormonal acne. I typically prescribe doxycycline 100mg daily or minocycline 100mg daily for 3-4 months maximum, always paired with topical treatments to prevent antibiotic resistance.
The goal is to use antibiotics as a bridge therapy while waiting for hormonal treatments or retinoids to kick in, then taper off.
Combined Oral Contraceptives (Birth Control Pills)
Birth control pills are incredibly effective for hormonal acne because they suppress ovarian androgen production and increase sex hormone-binding globulin (SHBG), which binds up free testosterone floating around in your bloodstream.
Four FDA-approved birth control pills for acne treatment contain ethinyl estradiol combined with:
- Norgestimate (Ortho Tri-Cyclen)
- Norethindrone (Estrostep)
- Drospirenone (Yaz, Yasmin)
- Drospirenone/ethinyl estradiol (Beyaz)
Expect to wait 2-3 months before seeing significant improvement. The combination pills work best for women who also want contraception, but they’re not suitable for everyone—women over 35 who smoke, those with a history of blood clots, or those with certain cardiovascular risks should avoid them.
Anti-Androgen Medications (Spironolactone)
Spironolactone is my go-to prescription for hormonal acne in women. This medication blocks androgen receptors on oil glands and reduces androgen production by the adrenal glands. It’s incredibly effective—studies show 50-100% reduction in acne for most women.
I typically start patients at 50mg daily and increase to 100-150mg if needed. You’ll notice decreased oiliness within a few weeks, but full acne clearance takes 3-6 months.
Important considerations:
- You must use reliable birth control while taking spironolactone due to potential birth defects
- Initial side effects include more frequent urination, breast tenderness, and irregular periods
- Avoid high-potassium foods and supplements (goodbye, coconut water)
- Monthly blood tests aren’t necessary for healthy young women
Isotretinoin (Accutane) for Severe Cases
Isotretinoin is nuclear-level acne treatment—and I mean that in the best way for severe, scarring hormonal acne that hasn’t responded to other treatments. It works by shrinking sebaceous glands, reducing oil production by 70-80%, and has anti-inflammatory effects.
The typical course is 0.5-1mg/kg daily for 4-6 months, aiming for a cumulative dose of 120-150mg/kg. Lower-dose regimens (20mg daily or even alternate-day dosing) are becoming popular for adult women with moderate hormonal acne, offering fewer side effects while maintaining effectiveness.
The reality check:
- Side effects include dry skin, chapped lips, joint pain, and potential mood changes
- Requires monthly pregnancy tests and reliable contraception
- Blood tests monitor liver enzymes and cholesterol levels
- Not recommended if you’re planning pregnancy within 6 months
Despite the downsides, isotretinoin can provide lasting remission from hormonal acne, especially when combined with maintenance therapy afterward.
When to Consider Oral Medications
Oral medications make sense when:
- Your acne is moderate to severe
- Topical treatments haven’t worked after 3 months
- You’re developing acne scars
- Your acne significantly impacts your quality of life
- You have signs of hormonal imbalance (irregular periods, PCOS)
Hormonal Therapy Options
How Hormonal Therapy Works
Hormonal therapy tackles acne at its source by reducing androgen production, blocking androgen receptors, or increasing estrogen to create a more favorable hormone ratio. Unlike topical treatments that address surface symptoms, hormonal therapy rewires your internal chemistry for long-term control.
Spironolactone: Dosage, Benefits, and Side Effects
I’ve already covered spironolactone above, but let me emphasize this: it’s one of the most effective treatments for hormonal acne in women, with minimal side effects when properly managed. The key is patience—stick with it for at least 4-6 months before judging results.
Typical side effects resolve within the first few months:
- Increased urination (take it in the morning to avoid nighttime bathroom trips)
- Breast tenderness
- Irregular periods initially
- Occasional lightheadedness
Most women tolerate spironolactone beautifully and can stay on it for years as maintenance therapy.
Birth Control Pills for Acne Treatment
Beyond the FDA-approved options mentioned earlier, many dermatologists prescribe other combination pills off-label for acne. The key is choosing formulations with low-androgen or anti-androgen progestins.
Avoid progestin-only pills (mini-pills) and contraceptives containing norgestrel or levonorgestrel—these have androgenic activity and can worsen hormonal acne.
Cyproterone Acetate and Other Options
Cyproterone acetate (CPA) combined with ethinyl estradiol is popular in Europe and Canada for treating hormonal acne. It has strong anti-androgen effects but carries a slightly higher risk of blood clots compared to other birth control options.
Flutamide is another anti-androgen occasionally used off-label but carries liver toxicity risks that make it a less popular choice.
Who Should Consider Hormonal Therapy?
Hormonal therapy is ideal for women who:
- Have acne concentrated along the jawline and lower face
- Experience premenstrual acne flares
- Haven’t responded adequately to topical treatments
- Have signs of hormonal imbalance or PCOS
- Want long-term acne control
- Need contraception anyway

Natural and Home Remedies for Hormonal Acne
Tea Tree Oil
Tea tree oil at 5% concentration has demonstrated antimicrobial and anti-inflammatory properties comparable to 5% benzoyl peroxide, though it works more slowly. Dilute essential tea tree oil with a carrier oil (jojoba or grapeseed) before applying as a spot treatment.
Green Tea Extract
Topical green tea extract reduces sebum production and has anti-inflammatory effects thanks to its polyphenol content. Some studies show drinking 2-3 cups of green tea daily may also help, though the evidence is limited. Look for skincare products containing at least 2% green tea extract.
Alpha Hydroxy Acids (AHAs)
AHAs like glycolic acid and lactic acid exfoliate dead skin cells, preventing pore blockage. They’re particularly helpful for comedonal acne and post-inflammatory hyperpigmentation. Start with 5-10% concentrations and work up gradually.
Zinc and Vitamin Supplements
Zinc (30-40mg daily) has anti-inflammatory properties and may help reduce acne severity. Studies show mixed results, but many of my patients report improvement.
Vitamin D deficiency correlates with acne severity in some studies. If you’re deficient, supplementing to normal levels might help reduce inflammation.
Omega-3 fatty acids (EPA and DHA) have anti-inflammatory effects and may reduce IGF-1 levels. Take 1000-2000mg daily from high-quality fish oil.
Probiotics for Skin Health
The gut-skin axis is real. Probiotic supplements containing Lactobacillus and Bifidobacterium strains may reduce systemic inflammation and improve skin barrier function. While research is still emerging, many women report clearer skin after adding probiotics to their routine.
Limitations of Natural Remedies
Let me be brutally honest: natural remedies rarely clear moderate to severe hormonal acne on their own. They work best as complementary treatments alongside medical therapy or for very mild cases. If you’ve struggled with hormonal acne for months without improvement, skip the Pinterest remedies and see a dermatologist.
Diet and Hormonal Acne
High-Glycemic Foods and Insulin Resistance
High-glycemic foods (white bread, sugary cereals, pastries, white rice) cause blood sugar spikes that trigger insulin release. Elevated insulin increases androgen production and stimulates IGF-1, both of which promote acne formation.
Research consistently shows that people eating high-glycemic diets have more severe acne compared to those eating low-glycemic diets rich in whole grains, vegetables, and lean proteins.
Dairy Products and Hormones
The dairy-acne connection is controversial but increasingly supported by research. Skim milk appears to be the worst offender, possibly because:
- Dairy contains natural hormones and growth factors
- Processing concentrates bioactive molecules
- Milk proteins may trigger inflammatory responses
If you suspect dairy triggers your breakouts, try eliminating it for 4-6 weeks and see what happens. Greek yogurt and hard cheeses seem to be better tolerated than milk and ice cream.
Foods That Help Reduce Acne
Anti-inflammatory foods to embrace:
- Fatty fish (salmon, sardines, mackerel)
- Leafy greens (spinach, kale, arugula)
- Berries (blueberries, strawberries)
- Nuts and seeds (walnuts, chia, flax)
- Green tea
- Turmeric and ginger
Anti-Inflammatory Foods and Omega-3 Fatty Acids
Omega-3 fatty acids from fish and plant sources reduce inflammatory mediators that contribute to acne. Studies show people who consume more omega-3s have less severe acne compared to those eating omega-6-heavy Western diets.
Foods and Supplements to Avoid
Beyond high-glycemic foods and dairy, watch out for:
- Whey protein supplements (highly insulinogenic)
- Excessive iodine from seaweed or supplements
- Vitamin B12 supplements (may worsen acne in some people)
- Branched-chain amino acid (BCAA) supplements
Comparison Table: Acne-Friendly vs. Acne-Triggering Foods
| Acne-Friendly Foods | Acne-Triggering Foods |
| Wild salmon | White bread |
| Quinoa | Sugary cereals |
| Sweet potatoes | French fries |
| Berries | Candy and cookies |
| Leafy greens | Skim milk |
| Walnuts | Whey protein shakes |
| Green tea | Soda |
| Lentils | White rice |
Skincare Routine for Hormonal Acne
Choosing the Right Cleanser
Forget harsh, stripping cleansers—they’ll only irritate your skin and trigger more oil production. Look for gentle, pH-balanced cleansers that remove dirt and oil without destroying your skin barrier.
Great options:
- CeraVe Foaming Facial Cleanser (for oily skin)
- La Roche-Posay Toleriane Hydrating Gentle Cleanser (for sensitive skin)
- Neutrogena Ultra Gentle Daily Cleanser
Wash your face twice daily, but don’t over-cleanse—this strips natural oils and paradoxically increases sebum production.
Moisturizers for Acne-Prone Skin
Even oily, acne-prone skin needs moisturizer. Using acne treatments without moisturizer damages your skin barrier, leading to increased sensitivity, inflammation, and—ironically—more breakouts.
Look for lightweight, non-comedogenic moisturizers with ingredients like:
- Hyaluronic acid (hydration without heaviness)
- Niacinamide (reduces oil and inflammation)
- Ceramides (repairs skin barrier)
My favorites:
- CeraVe PM Facial Moisturizing Lotion
- La Roche-Posay Effaclar Mat
- Neutrogena Hydro Boost Water Gel
Non-Comedogenic Products
“Non-comedogenic” means the product won’t clog pores. This label matters for everything touching your skin: moisturizers, sunscreens, makeup, and even hair products that might transfer to your face.
Avoid heavy oils like coconut oil, mineral oil, and petroleum jelly on acne-prone skin.
Sun Protection and Sunscreen
This is non-negotiable: wear broad-spectrum SPF 30+ sunscreen daily. Retinoids and many acne medications increase sun sensitivity, and UV exposure worsens post-inflammatory hyperpigmentation.
Choose mineral sunscreens with zinc oxide or titanium dioxide if chemical sunscreens break you out. Great options include:
- EltaMD UV Clear Broad-Spectrum SPF 46
- La Roche-Posay Anthelios Clear Skin Dry Touch Sunscreen
- CeraVe Hydrating Mineral Sunscreen
Exfoliation Best Practices
Chemical exfoliation with AHAs or BHAs (like salicylic acid) 2-3 times weekly helps prevent clogged pores. Skip physical scrubs—they cause microtears and inflammation.
If you’re using tretinoin or another strong retinoid, you might not need additional exfoliation.
Professional Treatments and Procedures
Chemical Peels
Professional chemical peels using salicylic acid, glycolic acid, or TCA can improve hormonal acne and fade post-inflammatory hyperpigmentation. A series of 4-6 peels spaced 2-4 weeks apart typically yields the best results.
Salicylic peels penetrate oil-filled pores particularly well, making them ideal for hormonal acne.
Cortisone Injections for Cystic Acne
Nothing shrinks a painful cystic pimple faster than a cortisone injection. Within 24-48 hours, inflammation dramatically decreases. I offer these for special occasions (weddings, important presentations) or particularly stubborn cysts that won’t resolve on their own.
The downside? Over-injecting can cause temporary skin depression, so this should be used judiciously.
Laser and Light Therapy
Laser and light-based treatments show promise for hormonal acne, though results vary:
- Blue light therapy kills acne bacteria
- Red light therapy reduces inflammation
- Photodynamic therapy (PDT) combines light with a photosensitizing agent for deeper effects
These treatments work best as adjuncts to medical therapy, not replacements.
Extraction of Comedones
Professional comedone extraction clears stubborn blackheads and whiteheads that won’t respond to topical treatments. Never attempt this at home—improper extraction causes scarring and worsens inflammation.
Microdermabrasion
Microdermabrasion provides superficial exfoliation that can improve skin texture and mild scarring. It’s not particularly effective for active hormonal acne but works well for post-acne hyperpigmentation.
How to Prevent Hormonal Acne Breakouts
Stress Management Techniques
Chronic stress elevates cortisol, which increases androgen production and triggers acne flares. Incorporate stress-reduction strategies:
- Regular exercise (but shower immediately after)
- Meditation or mindfulness practice
- Adequate sleep (7-9 hours)
- Therapy or counseling if needed
- Time for hobbies and relaxation
Sleep and Hormonal Balance
Sleep deprivation disrupts hormonal balance, increases cortisol, and impairs skin barrier function. Adults need 7-9 hours of quality sleep for optimal hormonal regulation and skin health.
Establish a consistent sleep schedule, avoid screens before bed, and create a dark, cool sleeping environment.
Skincare Habits to Avoid
Stop doing these acne-triggering habits:
- Picking, popping, or squeezing pimples
- Using dirty makeup brushes and pillowcases
- Touching your face throughout the day
- Applying too many products at once
- Using comedogenic hair products
- Skipping sunscreen
Maintenance Therapy After Treatment
Once your hormonal acne clears, don’t stop treatment abruptly. Maintenance therapy prevents relapse and includes:
- Continued use of topical retinoids or azelaic acid
- Ongoing hormonal therapy (spironolactone or birth control)
- Consistent skincare routine
- Healthy lifestyle habits
When to See a Dermatologist
Signs You Need Professional Help
Schedule a dermatology appointment if:
- Over-the-counter products haven’t worked after 8-12 weeks
- You have painful, deep cystic acne
- Your acne is causing scarring or hyperpigmentation
- Breakouts significantly impact your quality of life or mental health
- You suspect hormonal imbalance (irregular periods, excessive hair growth)
- You’re pregnant or planning pregnancy and need safe treatment options
What to Expect at Your Appointment
Your dermatologist will examine your skin, discuss your medical history, review current medications and supplements, and ask about your menstrual cycle and any symptoms suggesting hormonal imbalance.
Come prepared to discuss what treatments you’ve tried and how long you used them.
Laboratory Tests and Hormone Evaluation
If you have signs of hyperandrogenism (irregular periods, hirsutism, hair loss), your dermatologist may order blood tests:
- Total and free testosterone
- DHEA-S (dehydroepiandrosterone sulfate)
- LH (luteinizing hormone) and FSH (follicle-stimulating hormone)
- Fasting glucose and insulin (to screen for insulin resistance)
These tests should be done during the follicular phase of your cycle (days 1-5) between 8-10 AM for accuracy.
Questions to Ask Your Dermatologist
Helpful questions include:
- What’s causing my hormonal acne?
- Which treatment do you recommend and why?
- How long before I see results?
- What are the potential side effects?
- Do I need lab work or follow-up appointments?
- Can I use this treatment if I’m planning pregnancy?
- What’s my long-term maintenance plan?
Resource: American Academy of Dermatology – Acne Treatment
Treatment Timeline and Expectations
How Long Does Treatment Take?
Patience is crucial with hormonal acne treatment:
- Topical retinoids: 12 weeks minimum for visible improvement
- Oral contraceptives: 2-3 months
- Spironolactone: 3-6 months for full effect
- Isotretinoin: 4-6 months of treatment, with results lasting years
The “purge” period during the first 4-6 weeks of retinoid use is normal—your skin is clearing out existing microcomedones. Push through it.
Managing Side Effects
For retinoid irritation:
- Start with pea-sized amount every third night
- Buffer with moisturizer
- Gradually increase frequency
- Use SPF religiously
For spironolactone:
- Take with food to minimize stomach upset
- Schedule morning doses to avoid nighttime bathroom trips
- Stay hydrated
Preventing Acne Scars
Prevention is key because treating scars is harder than preventing them:
- Never pick or pop cystic acne
- Treat breakouts promptly with appropriate medications
- Use sunscreen to prevent hyperpigmentation
- Consider cortisone injections for large cysts
- Start professional treatments early if scarring develops
Long-term Management Strategies
Hormonal acne is often a chronic condition requiring ongoing management. Most women need to continue some form of treatment—whether topical retinoids, spironolactone, or birth control—to maintain clear skin.
Work with your dermatologist to find the minimal effective maintenance regimen that keeps your skin clear without unnecessary medication.
Special Considerations
Hormonal Acne During Pregnancy
Pregnancy severely limits treatment options since most effective acne medications are contraindicated:
Safe options include:
- Azelaic acid
- Topical erythromycin
- Benzoyl peroxide (short-term, low concentration)
- Glycolic acid peels
Avoid these:
- All retinoids (highly teratogenic)
- Spironolactone
- Tetracycline antibiotics
- Salicylic acid at high concentrations
Always consult your OB-GYN before starting any acne treatment during pregnancy.
Hormonal Acne and Menopause
Declining estrogen during perimenopause and menopause shifts the androgen-to-estrogen ratio, triggering hormonal acne in women who never struggled before.
Treatment often involves topical retinoids plus either spironolactone or hormone replacement therapy (HRT), which can address both acne and menopausal symptoms.
Treatment for Different Skin Types and Tones
For darker skin tones: Post-inflammatory hyperpigmentation is the primary concern. Prioritize:
- Azelaic acid (fades dark spots)
- Chemical sunscreen daily
- Gentle retinoids (start slow to avoid irritation)
- Avoid aggressive treatments that trigger inflammation
For sensitive skin: Choose gentler formulations:
- Adapalene over tretinoin
- Lower benzoyl peroxide concentrations (2.5%)
- Fragrance-free, minimal ingredient products
- Slow introduction of new actives
Men and Hormonal Acne
While less common, men can develop hormonal acne during puberty or if using testosterone supplementation for bodybuilding or hormone replacement.
Treatment for men typically focuses on topical retinoids and benzoyl peroxide rather than anti-androgens like spironolactone (which can cause gynecomastia in men).
Conclusion
Learning how to treat hormonal acne isn’t about finding one miracle product—it’s about understanding your unique hormonal landscape and building a comprehensive treatment plan that addresses the root cause. Whether you start with prescription retinoids and spironolactone, adjust your diet to reduce inflammatory triggers, or work with your dermatologist to optimize birth control options, the key is consistency and patience.
Hormonal acne may be stubborn, but it’s absolutely treatable. Most women see significant improvement within 3-6 months of starting appropriate therapy, though some need ongoing maintenance to prevent relapse. Don’t suffer in silence or waste money on products that can’t possibly work for hormonal breakouts. Work with a board-certified dermatologist who understands the complexities of adult female acne, commit to your treatment plan even when progress feels slow, and remember that clear skin is not just possible—it’s achievable.

